Insights
Demystifying the Medication Use Process
An Overview of the Medication Use Process
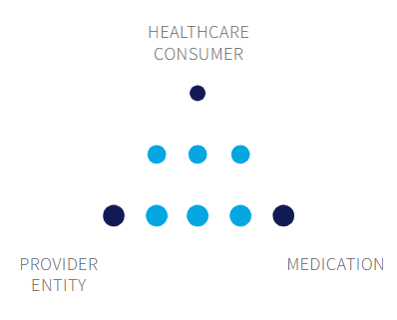
RevityRx’s medication use process (MUP) model illustrates the interdependent relationships between the stakeholders or nodes involved in the process. The nodes are Provider Entities, Healthcare Consumers, and the Medication. The model aims to simplify the complex MUP and establish a mutual understanding of the nodes at a high level. For a greater appreciation of the process complexity, exploration into each node’s composition will identify MUP levers to transform a siloed collection of activities into a comprehensive medication stewardship framework. This Insight provides an overview of the activities that comprise the MUP in acute and ambulatory settings and their relationship to RevityRx’s capabilities.
MUP Activities
The MUP is the sum of administrative, clinical, and operational activities beyond dispensing that result in a patient receiving medication to treat a health condition. This process begins with a physician or advanced practice clinician (APC) selecting a medication to the education and monitoring of a patient throughout treatment, inclusive of the financial aspect of payment for service. The overall process is complex and nuanced dependent on the healthcare setting where care is delivered and the acuity of the patient’s health condition.
Identification of specific MUP activities across acute and ambulatory sites of care assists an entity with identifying value-added opportunities to advance the medication use process and revitalize care standardization efforts.
| MUP Activity * | Details |
| Care Management | Care continuity activities in the ambulatory setting aimed at optimization or completion of medication therapy. Processes within care management focus on medication adherence monitoring, medication affordability, access, and availability. |
| Formulary Design and Methodology | Formulary process activities, primarily in the acute care setting, that range from formulary structure design to medication evaluation and subsequent value analysis. Processes consider subject matter experts and entity stakeholders relative to specialty area, site of care and overarching governance. |
| Governance | Compilation of administrative activities defining committee and subcommittee development and composition responsible for oversight of the clinical, administrative, and operational functions of the MUP. |
| Systems Optimization | Development or optimization of electronic medical record (EMR) tools and workflows that automate or streamline MUP activities enhancing dissemination of clinical and operational information. |
| Marketplace surveillance | Comprehensive process that couples monitoring regulatory agencies, professional organizations, or the lay media outlets for medication safety, availability, and healthcare financing updates with activities to address impact on MUP in acute and ambulatory settings. |
| Measures and Metrics | Development, collection and evaluation of process and outcome measures and metrics related to medication use. |
| Medication Reconciliation | Medication reconciliation activities that support the process of verifying and clarifying allergy information and creating the best possible medication list (BPML) a patient is taking or should be taking. The process includes a physician or APC comparing the medications a patient should be using (and is actually using) to the new medications that are ordered for the patient at every encounter and resolving any discrepancies. The process concludes with the transmittal of information to the appropriate caregivers. |
| Payer Liaison | Provider/payer relationship management and contracting activities primarily focused on value-based care agreements in the ambulatory care setting. Processes include continual review of cost, utilization, and quality metrics across the attributed payer's member population and design of actions to satisfy contract metrics. |
| Regulatory and Accreditation Compliance | Design, implementation, and coordination of activities to support compliance with accreditation requirements in accordance with MUP standards, policies, and procedures. |
| Staff Development | Design or revision of job descriptions, staff education, and competency assessments. |
| Therapeutic Management | Development of condition specific evidence-based guidelines that aim to improve patient outcomes. Therapeutic management activities incorporate standardized practices surrounding medication selection, monitoring, patient education and ongoing patient-centered medication optimization. |
| Transitional Care Management | Discharge planning and care continuity activities in the acute and subacute care settings, that prepare a patient to successfully transition to an ambulatory setting. Processes focus on medication affordability, medication availability, medication access, and enhanced post-discharge medication follow-up. |
| Workflow Optimization | Design and optimization of day-to-day clinical and operational activities aimed at creating high reliability within the MUP. Focused on the tenet of having the right role, doing the right work, in the right setting, at the right time to ensure safe and efficacious medication use and a positive experience for MUP stakeholders. |
* MUP Activities listed alphabetically.
MUP Activity Domains
All MUP activities are critical to an entity’s success in advancing the medication use process. RevityRx further groups these activities into four main domains: Clinical Program Optimization, Organizational Transformation, Resource Optimization, and External Stakeholder Integration.
Clinical Program Optimization focuses on establishing quality driven evidence-based solutions to foster cohesive comprehensive care. This may include the development of therapeutic guidelines, formulary design and methodology or transitional care continuity workflows.
Organizational Transformation focuses on an entity’s unique structure and culture to align strategy, define objectives, and establish medication use process metrics to achieve medication-related population health and healthcare consumerism goals.
Resource Optimization unlocks value in the medication use process by revitalizing staff training and competency and optimizing workflow design with the proper integration of vendor systems, tools, and information technology to enhance efficiency and engagement.
External Stakeholder Integration focuses on developing strategies and tactics to navigate regulatory and accreditation requirements, vendor relationship management and selection, marketplace insights, and payer and provider liaison based on the entity’s role in the medication use process.

